What are some of the symptoms and ailments that allow for a Medical Marijuana recommendation or Green Card.
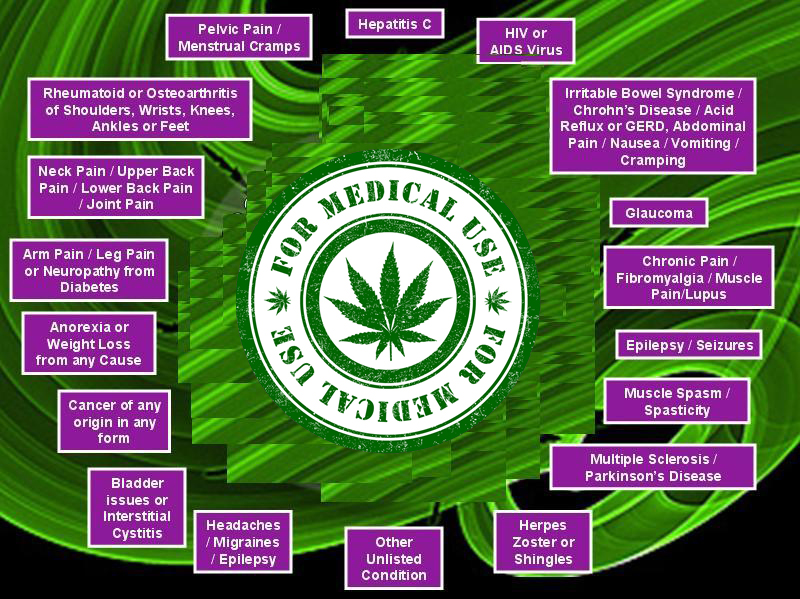
Click on Condition Above for What Records are Needed.
► Certificate of Recommendation
Alternative treatment has been approved by the State of Washington for use in various medical conditions. RCW 69.51A allows physicians to provide a “Certificate of Recommendation” to patients who qualify.
Common conditions the Department of Health has approved for the Certificate of Recommendation for include the side effects of Hepatitis-C, HIV infection, Chronic Pain conditions such as Arthritis in Joints, Degenerative Disc Disease of the spine, Inflammatory Bowel conditions such as Crohn’s Disease and Ulcerative Colitis, Nausea from any cause including chemo-therapy, Appetite and Weight Loss, Headaches and Migraines, Seizures-Epilepsy, Multiple Sclerosis, Abdominal Cramping, Fibromyalgia, Severe-Intractable Pain from any cause, side-effects from Cancer, Sleep Disorders and Glaucoma as well as other medical conditions.
If you do not have your medical records in your possession, contact your treating doctors so they can be faxed directly to our office. Please do not send double sided or reduced chart notes as the records will not be reviewed.
If you cannot fax your medical records mail them directly to our office at: Dr. Havsy 3716 Pacific Ave, Suite E Tacoma, WA 98418.
If your condition is not listed or you have any questions feel free to call our office at 425-276-6640.
Once your records are received, they are logged-in and a staff doctor reviews the records typically within 7-10 business days. If additional records are required, our staff will contact you and provide you with the information that is required.
Once approved, you will notified by our staff at the phone number you provided. A NON-REFUNDABLE deposit is required before your appointment is scheduled. We accept money orders, cash or credit cards only. If you fail to keep your appointment or do not provide a 48 hour notice of cancellation, your deposit will be forfeited and another deposit will be required to reschedule your appointment.
PLEASE NOTE:
- Do not send in double sided copies of records for review.
- Records sent are the property of Dr. Havsy whether or not you are approved for a certificate of use.
- If you are approved, your records will then become part of your permanent medical file in our office.
- If you are not approved, the records will be destroyed. Therefore, do not send original records or records that you do not have copies of and expect to get back.
- If you fail to keep your appointment or do not cancel within 48 hours, your deposit fee will be forfeited.
► Neck pain, upper back pain, low back pain, joint pain of the shoulder, elbow, wrist, hip, knee, ankles or feet:
- CT scans, MRI scans, and X-ray reports of the area in question.
- Orthopedic or neurosurgical consult
- Procedures such as spinal injections, or nerve studies
- Surgery reports of the area in question
- 4 treatment records or notes from a physician’s office indicating treatment to that specific area within the last two years.
► Rheumatoid or osteoarthritis of the shoulders, elbows, wrists, hips, knees, ankles or feet:
- Evaluation from an orthopedic, neurosurgeon or rheumatologist
- Blood tests indicating you have rheumatoid arthritis.
- CT scans, MRI scans, and X-ray reports of the affected area.
- Treatment records or notes from a physician’s office indicating treatment to that specific area within the last two years.
► Hepatitis C:
- Blood tests that show you have Hepatitis C or a viral load of hepatitis.
- Liver biopsies
- Gastroenterology consult
- MRI, CT scans or Ultrasound of the liver.
- Four treatment notes indicating that you have Hepatitis C from any treating physician over the past 2 years.
► HIV or AIDS virus:
- Blood test that show you have the AIDS virus.
- 4 treatment notes with infectious disease doctor or from a physician who is currently treating your condition over the past 2 years.
► Irritable bowel syndrome/gastro esophageal reflux or GERD, abdominal pain:
- Gastroenterology consult
- CT/MRI/Ultrasound of abdomen
- Endoscopy of stomach or colonoscopy report
- Upper or lower GI barium tests
- Four treatment notes reflecting your medical condition over the past 2 years
► Headaches/migraines/epilepsy:
- Neurological consult
- CT scan or MRI of the brain
- EEG
- Four treatment notes from neurologist or primary care physician reflecting treatment for this condition over the past 2 years
► Bladder issues or interstitial cystitis:
- Urology consult
- Recent urinalysis
- Surgery report/cystoscopy of bladder
- Four treatment records from your primary care physician or specialist indicating you have interstitial cystitis over the past 2 years
► Cancer of any origin:
- Copy of consult with your cancer specialist
- Surgery reports that reference removal or attempted removal of your cancer
- Chemotherapy reports
- Four treatment notes from your specialist or primary care provider that indicate follow-up for cancer over the past 2 years
► Anorexia or weight loss from any cause:
- Gastroenterology consult with colonoscopy, endoscopy, upper or lower GI series
- Four treatment notes indicating anorexia or weight loss from your primary care doctor or specialist; or
- Psychiatric evaluation with four follow-up treatment notes
► Arm pain/leg pain/ or neuropathy from diabetes:
- Consult with your neurologist, orthopedic surgeon, neurosurgeon or rheumatologist, endocrinologist or hormone doctor
- Nerve conduction studies and electromyography/EMG studies of the upper or lower extremities
- Blood tests indicating you have diabetes
- CT scans or MRI scans of the neck or low back
► Glaucoma:
- Legible chart notes in the last two years that document your glaucoma with pressure readings, the diagnosis of glaucoma and what medication you are currently taking for that condition.
- As a vast majority of these records are handwritten, we may require a letter from your ophthalmologist indicating that you have been diagnosed with glaucoma and what your pressure readings were before you began the use of medication
► Herpes zoster shingles:
- Blood tests indicating you have herpes zoster or shingles
- Neurology consult, if any
- Nerve studies
- Four treatment notes from your primary care physician indicating your condition in the last 2 years
► Pelvic Pain / Menstrual Cramps:
- Evaluation by a gynecologist or medical physician
- Ultra Sound of Abdomen / pelvis / uterus
- Four treatment notes documenting your condition
► Chronic Pain / Fibromyalgia / Muscle Pain / Lupus:
- Rheumatology, orthopedic, neurologist or neurosurgeon evaluation.
- Copies of MRI scans, X rays, CT scans or affected areas
- Copies of blood tests that reflect you have fibromyalgia
- Four treatment notes from your doctor over the past 2 years that indicate you have fibromyalgia, chronic pain, muscle pain or Lupus
► Epilepsy / Seizures:
- Neurologist evaluation
- Copies of MRI scans or CT scans of the brain
- Copies of EEG's of the brain
- Four treatment notes from your doctor over the past 2 years that indicate you have seizures
► Muscle Spasm / Spasticity:
- Rheumatology, orthopedic, neurologist or neurosurgeon evaluation
- Copies of blood tests that reflect fibromyalgia
- Copies of any EMG or nerve studies
- Four treatment notes from your doctor over the past 2 years that indicate you have been treated for muscle spasm or spasticity
► Multiple Sclerosis or Parkinson's:
- Neurologist evaluation or Primary Care evaluation
- Copies of MRI scans or CT – scans of the brain
- Copies of spinal tap results
- Four treatment notes from your doctor over the past 2 years that indicate you have multiple sclerosis or Parkinson's
► Condition not listed:
Chronic Renal Failure
- Blood work indicating your kidneys do not function (BUN/Creatinine levels).
- Consult with Internal Medicine Doctor or Nephrologist (Kidney Doctor).
- 4 treatment notes in the last two years from your doctor who treated you for kidney failure.
Call our office for document information 425-276-6640
